|
Cancer, chemo, radiation, steroids, surgeries, the whole speal of this journey can leave your body in a wreck, a train wreck; a wreck that can take time to recover, maybe never even fully recover. ‘New normal' is what us in the cancer world call this. Finding your new normal is but another segment to the cancer journey. This can be incredibly challenging, even intimidating for many. Post-chemo can leave cancer survivors left hanging alone, an untraveled road, one that can lead into post-traumatic stress (PTSD). Yes,
post-traumatic stress is real and an entire topic alone (outside soldiers’ stories). Post-cancer treatment is often left unaddressed leaving cancer patients to find this new normal alone through trial and error. This can be dangerous, bringing frustrations to the added learning to live out the new normal of everything all
0 Comments
 As we all sit in our homes, isolated away from our normal day-to-day activities and peeps, to the cancer world, this is nothing new or unexpected. Us cancer survivors and patients know first-hand about homebound isolation and staying away from people. We know about having to leave our day to day activities to allow for treatments, appointments, tests, resting, healing or just doing nothing but breathe. We know what it is like to have our entire life come to a halting stop. We know what it’s like to be sitting within our walls, watching from the inside. We know the ideas of confinement and withdrawals. We know the long-lived anticipation to return to normal, oh, yes, normal, a normal that many never get back to….we know all too well. We know what it’s like wearing masks all while eyeing people from afar. We know all too well the varied  That is a question, a question for many facing chemotherapy or currently on chemotherapy. A question for some of us post-chemo or those who have been left with more permanent side effects. You’re left with the decision of changing your look in order to look similar to how you did before treatment or styling differently according to your new situation. Whatever your reason to question, it is always smart to learn the pros and cons. You should never feel pressured to do one thing or the other. During my long, hard
How and when do you tell someone new about your cancer history? Yea. This topic has taken me to many uncomfortable zones, levels beyond my normal. This changed once I put myself in many of those uncomfortable zones.
It all started with a lack of information upon my diagnosis. This led me to social media. I was looking for All I heard over a 12 hour period was that I was pregnant and/or miscarrying across several floors--from the ER to Labor & Delivery to Telemetry--until they tried to send me home. The last remark I heard before an actual diagnosis was that I was having a heavy period. As I was hemorrhaging. We're talking two buckets full, nearly-passing-out, horror-movie stuff. This was not just a heavy period. Give me a break.
Repeatedly, I refused their explanations for my four-month-postpartum intermittent bleeding. Repeatedly, I refused to go home. I was NOT going to bleed to death in my bed. I knew something was wrong and that 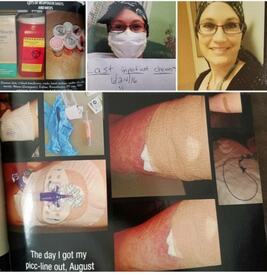 I remember the day clearly. My head was still rapidly spinning. I had finished weekly chemotherapy after six and a half months and my picc-line (peripherally inserted central catheter) was about to be removed. The reality was, I was terrified of this change. A number of what-if's filled my mind and uncertainties quarantined my body. So soon? I wasn't ready for this, yet it was an oncology order. I had learned to adjust to this being in my arm; it had been part of my arm as I learned to deal with the pain and minimal use that seeing it off was too much to grasp. I needed a little more time! The thought of my cancer returning and having another one put in was horrid. The picc-line RN that put it Bald is powerful. Bald is beautiful. Bald is bold. Bald is stylish. Bald is bald.
You may or may not agree with these. You may have had a change of heart as to how you see bald after your treatments. Maybe you don't. How do you see bald? For me, I saw bald very quickly. I had thinning hair on my first single agent treatment plan, but once I was Some are willing to talk about anxiety while others are not, remaining hidden beneath their fears and the torture of it. When my molar pregnancy disease progressed to aggressive malignant cancer choriocarcinoma, my anxiety was at its highest. A molar pregnancy is rare, and threatens the life of a child. In my case, this affected the twins I was expecting and in turn led to me getting cancer.
What is anxiety? Plainly put, it is stress, but it goes much deeper for many people; it can be internal fear, affecting everyday life, minute to minute, hour to hour. Typical signs are irregular heart palpitations, It's not everyday you get to stay in the hospital, and most hospitals are far from luxurious. However everyone at some point in their lifetime spends at least one visit in the hospital, whether it be surgery, illness, or cancer treatment. Let's face it-hospital time is boring. Time seems to move very slowly. What are some tips to help the time pass?
I have done my share of time in the hospital after being diagnosed with placental cancer, choriocarcinoma, |
Categories
All
|

